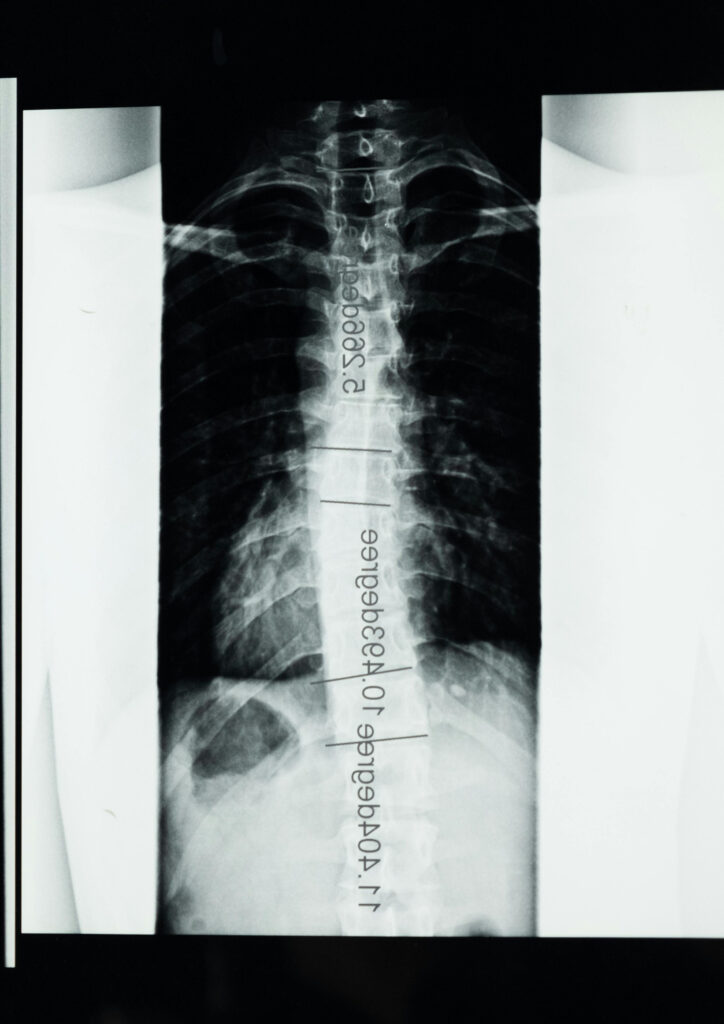
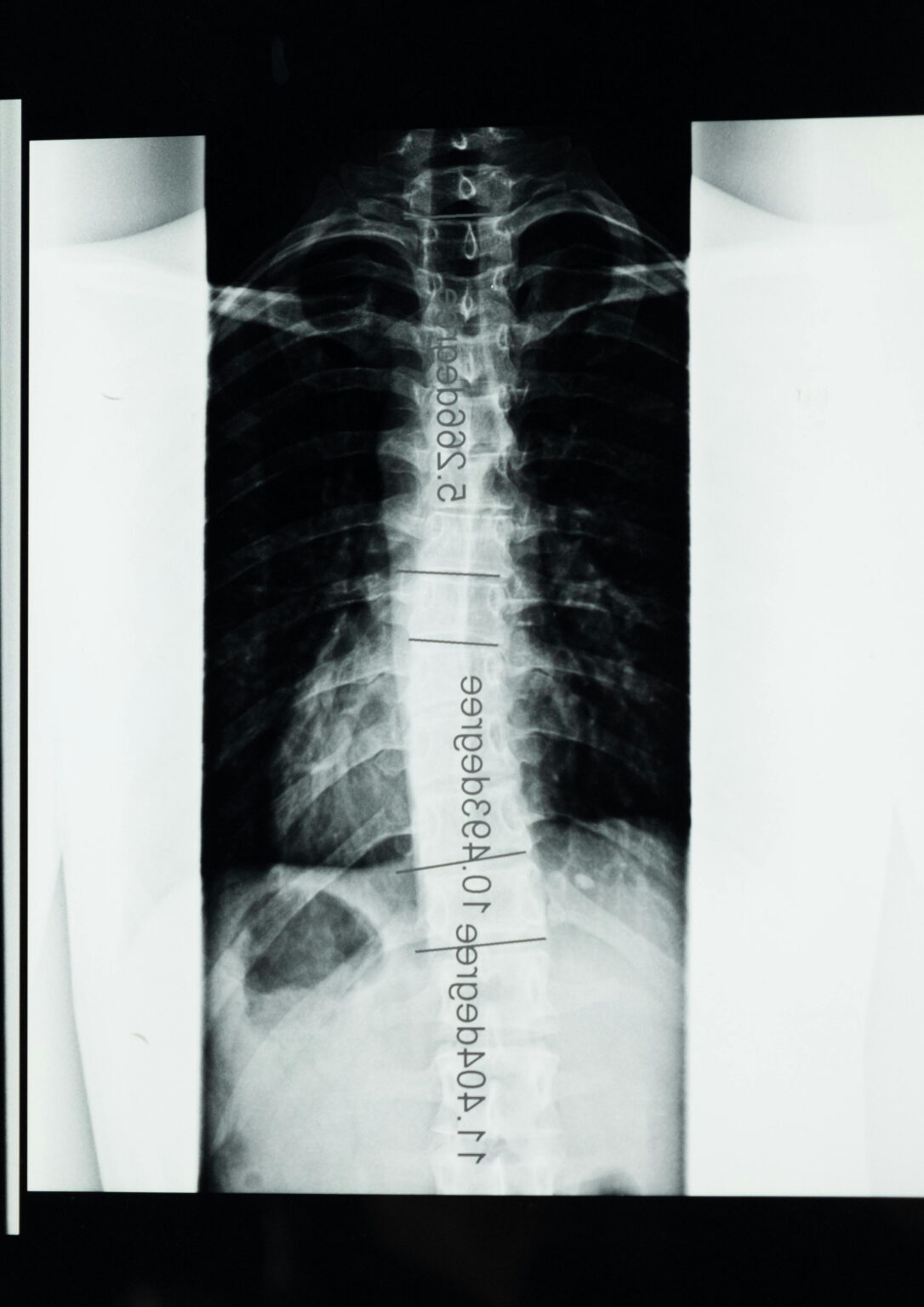
Spinal fusion surgery is a procedure that permanently joins two or more vertebrae (the individual small bones that stack together to form your backbone) to eliminate movement between them. By stabilising the affected segment of the spine, the surgery aims to reduce pain caused by abnormal motion and prevent further damage to surrounding spinal structures.
During the procedure, the neurosurgeon places bone graft material between the affected vertebrae. This graft may come from your own bone, a donor source, or a synthetic substitute. Over time, the bone graft heals and fuses the vertebrae into a single solid unit, providing long-term stability to the spine.