Navigating Brain Tumour Treatment in Singapore – How to Choose the Right Brain Surgeon
Our brains are at the core of everything we do—our thoughts, memories, movements, and even our emo
acf domain was triggered too early. This is usually an indicator for some code in the plugin or theme running too early. Translations should be loaded at the init action or later. Please see Debugging in WordPress for more information. (This message was added in version 6.7.0.) in /home/precisio/public_html/wp-includes/functions.php on line 6121
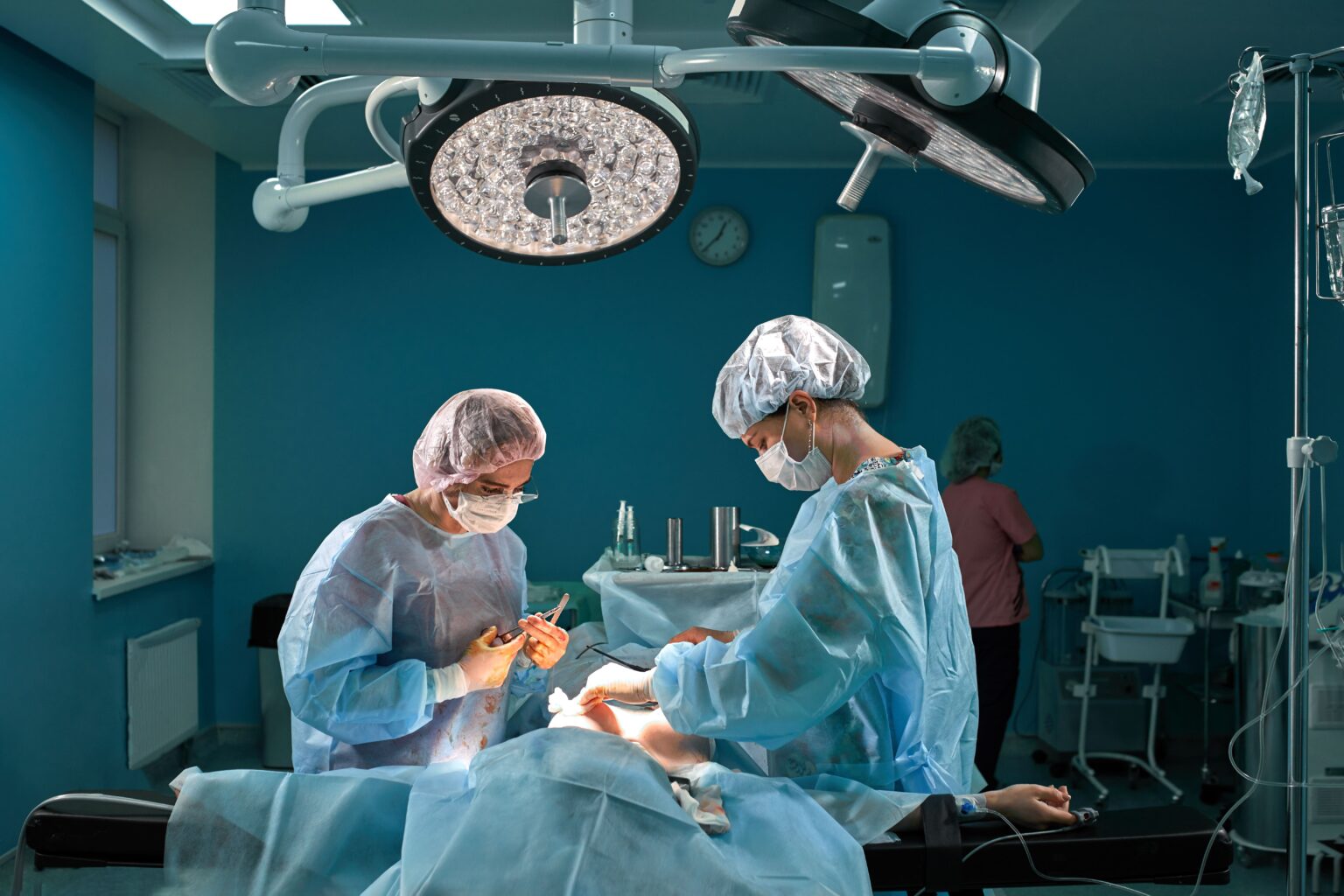
Beyond conventional surgical treatments, awake brain surgery presents the intersection of precision, real-time feedback, and medical innovation. In this blog, we will discuss the intricacies of awake brain surgery, exploring its transformative potential in treating complex brain conditions.
Awake brain surgery, also known as awake craniotomy, is a specialised surgical approach used to treat brain tumours, epilepsy, and other neurological conditions. Unlike conventional surgeries that are performed under general anaesthesia, awake craniotomy involves keeping the patient awake and alert during certain phases of the procedure. This allows the neurosurgeon to interact with the patient in real-time, enabling precise mapping and preservation of critical brain functions.
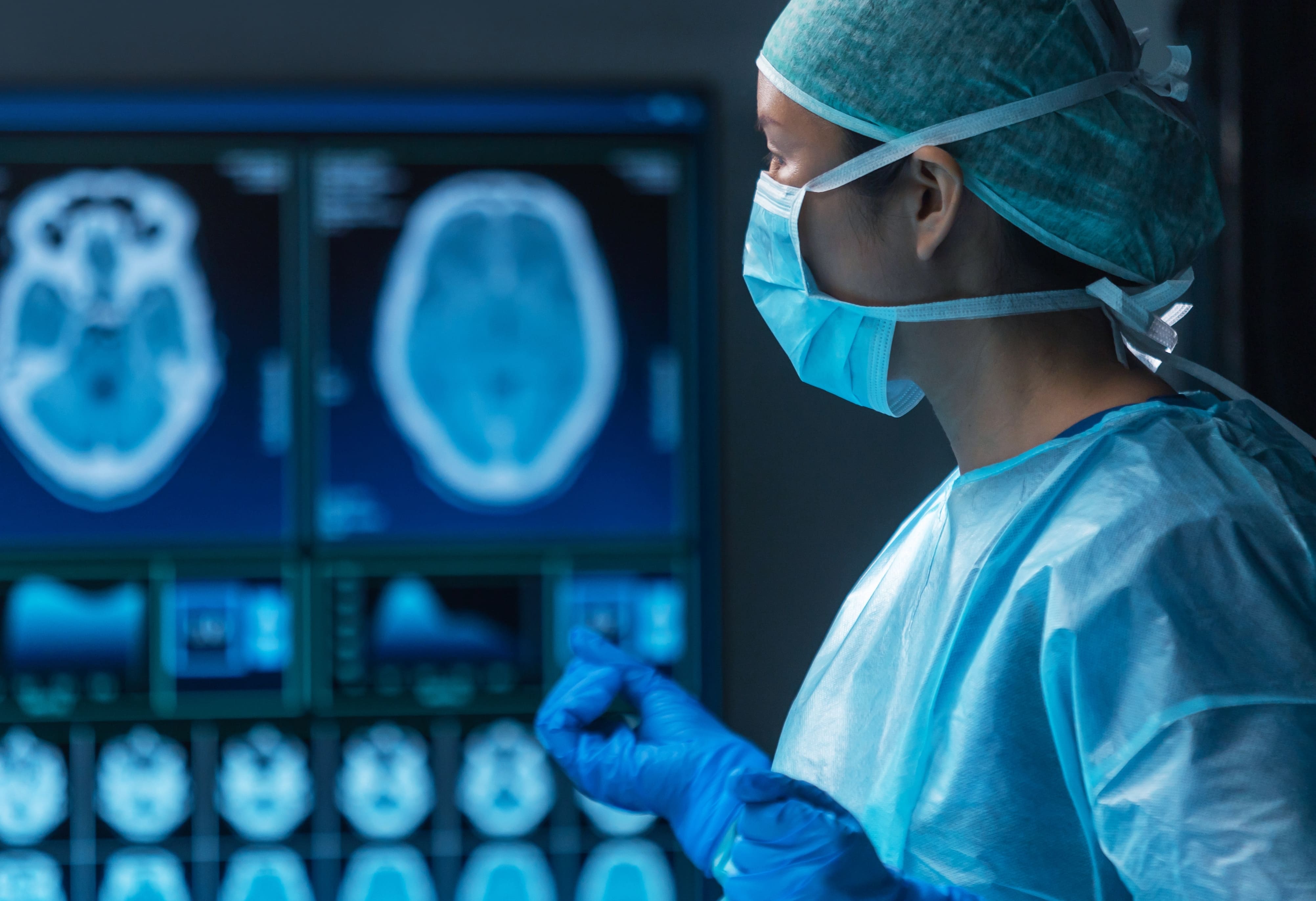
The process of awake craniotomy typically unfolds in several stages:
To begin the procedure, the patient is initially administered local anaesthesia followed by sedation to induce a state of unconsciousness. Once the skull is opened and the brain is exposed, the sedation is stopped to allow the patient to regain consciousness gradually.
With the patient awake, the neurosurgeon uses techniques such as direct electrical stimulation or functional MRI to map vital areas of the brain responsible for functions such as speech, movement, and sensation. During this process, patients are tasked with a series of tests guided by a neuropsychologist. These tasks include speaking, movement of objects, recalling information, and more. With real-time feedback as such, neurosurgeons can map out parts of the brain to ensure preservation of critical functions while removing or treating the targeted lesion.
With the brain mapped and critical areas identified, the neurosurgeon proceeds with the main objective of the surgery, whether it’s removing a tumour, treating epilepsy, or addressing other neurological conditions. Throughout this phase, the patient remains awake and responsive, providing invaluable feedback to the surgical team.
Once the surgical objectives are accomplished, the sedation is adjusted again to deepen the patient’s level of sedation for the closure of the incision and completion of the procedure.

While it may seem daunting to be awake for brain surgery, there are several advantages to this approach.
With the patient awake and responsive, the brain surgeon can distinguish between tumour tissue and healthy brain tissue with better accuracy. This facilitates maximal tumour removal while preserving critical functions such as language, speech, and motor skills.
The patient’s ability to communicate during surgery allows for immediate feedback on any changes in neurological function. This enables prompt adjustments to ensure mapped out regions are left untouched, minimising the risk of functional deficits.
Awake craniotomy allows the preservation of functionally essential brain regions such as motor functions, speech, memory and more. This ensures that patients can still retain the critical functions, maximising their quality of life post-surgery.
Awake brain surgery is used to treat any lesions including brain tumours, cavernomas, arteriovenous malformation (AVM), or regions that involve eloquent segments of the brain.
Staying awake during surgery can sound intimidating. However, awake brain surgery, also known as awake craniotomy, is a surgical procedure that aims to maximise tumour removal whilst preserving critical functions.
At Precision Neurosurgery, our director neurosurgeon Dr Teo Keija, has over 15 years of experience and specialises in brain mapping and awake brain surgery. He is well-equipped to treat brain, spine and certain nerve conditions.
Book an appointment here.
Consult with Dr Teo for a comprehensive evaluation and a personalised treatment plan.


Dr Teo Kejia is a Senior Consultant Neurosurgeon and Medical Director at Precision Neurosurgery, with more than 15 years of clinical experience.
Dr Teo has extensive knowledge and experience in the field of neurosurgery, with a particular focus on complex brain tumour procedures. He is adept in employing advanced surgical techniques, including brain mapping and awake brain surgery, especially for treating gliomas and glioblastomas. His expertise extends to neuro-oncology, encompassing both brain and spinal tumours, as well as neurovascular and skull base surgery.
Additionally, Dr Teo offers treatment for a range of neurological conditions, such as traumatic head injuries, intracerebral aneurysms, and degenerative spine disorders, which include neck and back pain. He is also proficient in managing ischemic and haemorrhagic strokes, hydrocephalus, trigeminal neuralgia, and hemifacial spasm.
Have a question or need more information? Please fill in the form below, and our team will assist you.